Fruits and vegetables and the risk of type 2 diabetes is there an association?
The global burden of diabetes is increasing, with the latest data from the International Diabetes Federation estimating a prevalence of 285 million in 2010, increasing to a staggering 439 million by 20301. The increased premature ill health, reduced life expectancy, and increased death rate related to the presence of diabetes, provide reason for concern, and make its prevention a major public health priority. That the primary prevention of diabetes is possible through lifestyle behaviours, including a healthy diet, has now been well established by intervention trials among people at high risk of diabetes2. However, what the specific contribution might be of the intake of fruits and vegetables to diabetes prevention, is unresolved.
We hypothesised that the inconsistent findings3-5 for an association between intake of fruit/vegetables and the risk of type 2 diabetes might be explained by the known imprecision and measurement error in assessing fruit/vegetable intake from selfreport methods such as the food frequency questionnaire. We thus aimed to examine the association of plasma vitamin C, an objective biomarker of fruit/vegetable intake, and the risk of future diabetes. We also examined the association of diabètes with self-reported fruit and vegetable intake.
The EPIC-Norfolk Study
The European Prospective Investigation of Cancer-Norfolk (EPICNorfolk) study is a population-based cohort study. Men and women aged 40-75 years, resident in Norfolk, U.K. were identified from family-doctor age-sex registers, and of 77,754 invited, 25,639 attended for a health check visit in 1993-97. Dietary intake was assessed by a semi-quantitative food frequency questionnaire and vitamin C was measured in blood (plasma) samples. After exclusions, 21,831 individuals (9,815 men; 12,016 women) were eligible for analysis. Participants were without known diabetes at baseline, and we ascertained new-onset diabetes (n=735) over 12 years of follow up6.
An association might be obscured by measurement error
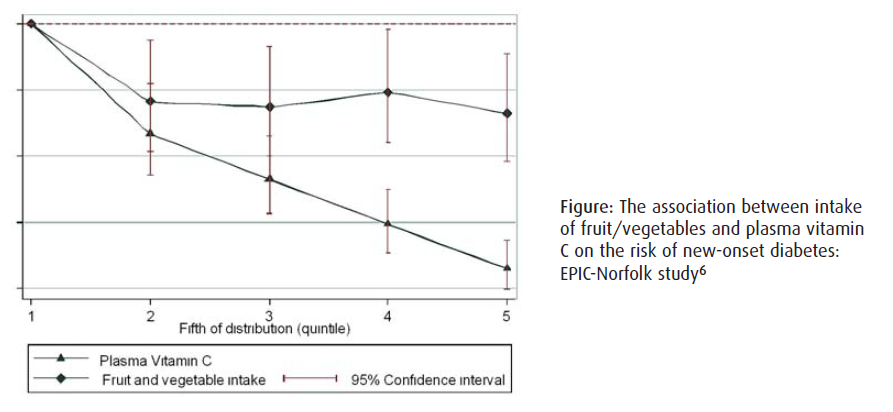
There was a striking inverse association between plasma vitamin C concentration and the risk of new-onset diabetes, while the association with total fruit/vegetable intake was modest, and lacked the ‘dose-response’ effect seen with plasma vitamin C (Figure)6. The risk of diabetes in the top fifth (compared to bottom fifth) of the plasma vitamin C distribution was 62% lower (95% confidence limits 48% to 72% lower), while for a similar comparison for fruit/vegetable intake there was a modest 22% reduction in risk of diabetes (95% confidence limits 0% to 40% lower risk). These analyses accounted for other factors, such as potential healthier lifestyles among those who eat greater quantities of fruit/vegetable or have higher vitamin C levels [adjusting for age, sex, family history of diabetes, lifestyle factors (alcohol intake, smoking, physical activity), socio-economic status (education, social class), obesity (body mass index and waist circumference), and intake of vitamin supplements].
Conclusions
Evidence for the benefits of greater intake of fruits/vegetables for diabetes prevention is elicited strongly and convincingly when plasma vitamin C (a valid biomarker) is used as a proxy for fruit and vegetable intake. In contrast, the same association is attenuated and more modest when self-reported fruit/vegetable intake is used. Because fruit and vegetables are the main source of vitamin C, these findings suggest that eating even a small quantity of fruit/vegetables may be beneficial and that the protection against diabetes increases progressively with the quantity of fruit and vegetables consumed.
References
- Shaw JE et al. [2010] Diabetes Res Clin Pract 87, 4-14.
- Gillies CL et al. [2007] Br Med 334, 299-307.
- Hamer M et al. [2007] J Hypertens 25, 2361-2369.
- Liu S et al. [2004] Diabetes Care 27, 2993-2996
- Bazzano LA et al. [2008] Diabetes Care 31, 1311-1317.
- Harding AH et al. [2008] Arch Intern Med 168,1493-1499.
