Health Behaviours From Early to Late Midlife as Predictors of Cognitive Function – The Whitehall II Study
Background
There is growing evidence of an association between health behaviours and cognitive ageing. Smoking, alcohol abstinence, lack of physical activity, and poor dietary behaviour has all been found to be associated with cognitive decline and dementia. Although prospective studies have shown individual health behaviours to be associated with cognition, their combined impact on cognition remains unexplored. The objective of the present study is to assess the association of individual health behaviours and their combination with poor cognition in late midlife. We used health behaviours assessed three times over a 17-year period to examine whether unhealthy behaviours, separately and together, are associated with poorer executive function and memory and whether the risk associated with unhealthy behaviours accumulate over the adult lifecourse.
The Whitehall II Study
The target population for the Whitehall II study was all London-based office staff, aged 35–55 years, working in 20 civil service departments. Health behaviours were assessed in early midlife (mean age=44 years, Phase 1, 1985-1988), in midlife (mean age=56 years, Phase 5, 1997-1999) and in late midlife (mean age=61 years, Phase 7, 2002-2004). Smoking status at the three phases was assessed using questions on current smoking behaviour; high risk was defined as being a “current” smoker. Alcohol consumption was assessed via questions on the number of alcoholic drinks (“measures” of spirits, “glasses” of wine, and “pints” of beer) consumed in the last seven days, converted to number of units of alcohol with each unit corresponding to eight grams of ethanol. Alcohol consumption was categorized as: no alcohol, 1-14 units, and 15 or more units of alcohol per week. Compared to moderate alcohol consumption (1-14 units/week), alcohol abstinence was associated with a higher risk of poor executive function and poor memory. As no increase in risk was found among participants who consumed more than 14 units per week, the high risk category was thus defined as “abstinence from alcohol” rather than excessive alcohol consumption1. In this cohort, heavy alcohol use was rare. Physical activity was assessed using questions on the frequency and duration of participation in different level of physical activities that were used to compute hours per Week of each intensity level. Low risk was defined at each of the three phases as more than 2.5 hours per week or more of moderate physical activity or one hour or more per week of vigorous physical activity (30). Dietary behaviour was assessed using a measure of frequency of Fruit and Vegetable (F&V) consumption. The low risk category was defined as eating F&V two or more times a day. A score of the number of unhealthy behaviours (smoking, alcohol abstinence, low physical activity, and low F&V consumption) was defined as ranging from 0 to 4. Poor (defined as scores in the worst sex-specific quintile) executive function (assessed using factor score of measures of reasoning (AH4-I) and phonemic and semantic fluency) and memory in late midlife (Phase 7) were analyzed as outcomes.
Association between health behaviours and cognitive deficit
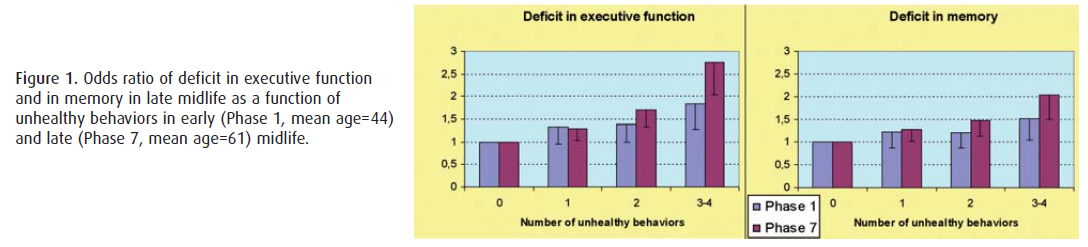
Each of the four unhealthy behaviours examined – smoking, alcohol abstinence, low physical activity, poor dietary behaviour – at any of the three measures over the 17-year follow-up was associated with poor executive function and memory in late midlife. Compared to those with no unhealthy behaviours, those with 3-4 unhealthy behaviours at Phase 1 (Odds Ratio (OR)=1.84; 95% Confidence Interval:1.27,2.65), Phase 5 (OR=2.38;1.76,3.22) and Phase 7 (OR=2.76;2.04,3.73) were more likely to have poor executive function. A similar association was observed for memory (Figure 1). Odds of poor executive function and memory were the greater the more times the participant reported unhealthy behaviours over the three phases.
Promotion of a healthy lifestyle is important for cognitive health
References
- Knoops KT, de Groot LC, Kromhout D, et al. JAMA 2004; 292(12): 1433-9
- Khaw KT, Wareham N, Bingham S, et al. PLoS Med 2008; 5(1): e12
- Yates LB, Djousse L, Kurth T, et al. Arch Intern Med 2008; 168(3): 284-90
- van Dam RM, Li T, Spiegelman D, et al. BMJ 2008; 337: a1440
- Chiuve SE, McCullough ML, Sacks FM, et al. Circulation 2006; 114(2): 160-7
- Kurth T, Moore SC, Gaziano JM, et al. Arch Intern Med 2006; 166(13): 1403-9
